 Hot Off the Press – October 28, 2019.
Hot Off the Press – October 28, 2019.
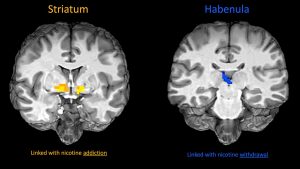
Approximately 1.1 billion people smoke cigarettes worldwide. More than half of these are expected to die of smoking-related diseases. According to the US Centers for Disease Control: most smokers (68%) want to quit; about half (54%) try to quit each year; yet very few (about 7%) do quit. One reason quitting smoking is so hard is the nicotine withdrawal symptoms smokers experience including: anxiety, irritability, difficulty concentrating and reduced pleasure. Nicotine withdrawal symptoms are linked with reduced activity in the brain’s reward processing (dopamine) system. Understanding differences in brain activity: 1) between smokers and nonsmokers, and 2) after getting medication treatment for smoking cessation is important for improving smoking treatments. In this study, scientists at NIDA and Florida International University gave 2 commonly used medications: nicotine and varenicline (Chantix ™) to nonsmokers and abstinent smokers. The scientists used functional Magnetic Resonance Imaging (fMRI) to measure brain activity when people played a game where they picked which item they thought would win a race across a computer screen. They got positive feedback when they were correct and negative feedback when they were wrong. This allowed the scientists to look at the brain’s reward processing system. They found that smokers showed lower brain activity to reward in a brain region called the striatum. The striatum is a major part of the brain’s reward processing system. The brain activity did not improve when smokers got either medication. Lower brain activity was linked to higher levels of addiction in the smokers and negative affect in both smokers and non-smokers. These results suggest that current smoking cessation medications do not help reward processing deficits in smokers. Such deficits may make pleasurable experiences less enjoyable. Conversely, the scientists also observed activity in the habenula following both positive and negative feedback that was linked with intensity of withdrawal symptoms and was reduced by nicotine but only in the smokers, indicating the effect was related to nicotine withdrawal. More habenula activity was linked with higher levels of craving. These results suggest that elevated habenula activity during withdrawal can be targeted by current smoking cessation treatments. Overall, these important results indicate that 1) current medications do not fix reward processing problems in smokers’ striatum (this might explain why many smokers continue to smoke while taking medications) but 2) the habenula is linked with nicotine withdrawal symptoms and it does respond to nicotine replacement.
Publication Information
In: Sci Adv, vol. 5, no. 10, pp. eaax2084, 2019, ISSN: 2375-2548 (Electronic); 2375-2548 (Linking).
